For Patients
Barrett's Oesophagus - Ablation Procedure with the HALO 360 System
"Removal of the Barrett's epithelium with Circumfrential Radio Frequency Ablation"
During the Procedure
Using standard endoscopy techniques, the physician activates and controls the different functions of the HALO360 System.
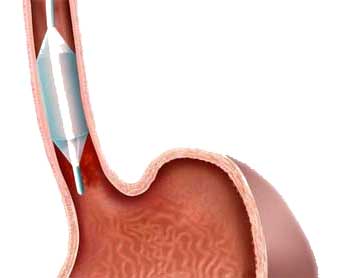
SIZING
- A catheter is inserted into the oesophagus along side the endoscope.
- At the tip of the catheter there is a small balloon that is inflated once inside your oesophagus near the treatment area. The balloon and the HALO360 Energy Generator together measure the diameter of your oesophagus. This information is used by the physician to select the appropriate treatment catheter.
- The sizing balloon is then removed and the treatment or HALO360+ Ablation Catheter is introduced.
|
 |
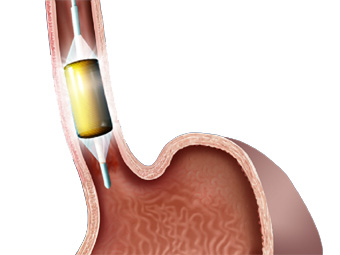 |
ABLATION
- The HALO360+ Ablation Catheter also has a balloon at the tip, but this balloon is covered by a band of radiofrequency electrodes.
- Once the electrodes of the balloon are positioned on the desired treatment area the balloon is inflated. The HALO360 Energy Generator and the ablation catheter then work together to deliver a short burst of energy that is circumferential: 360 degrees.
- The design of this technology limits the energy delivery to a depth clinically proven to remove the diseased tissue while reducing the risk of injury to the deeper healthy tissue layers
- The HALO360+ Ablation Catheter ablates a 3 cm circumferential segment of Barrett's tissue within the oesophagus
- For patients with Barrett's oesophagus lesions longer than 3 cm, the HALO360+ Ablation Catheter is simply repositioned and the ablation steps are repeated.
|
What to Expect After the Procedure
It is very important that a patient follows the discharge instructions provided by the physician or the nursing staff after the procedure to ensure limited time of discomfort and ensure proper healing of the oesophagus. Clinical studies show that re-growth of healthy tissue occurs within one month in the treated area.
The studies also demonstrated that patients had 90% of their Barrett's removed after one or two treatment sessions at one year follow-up. In addition the studies showed that over 70% of the patients were completely cured of their Barrett's after 1 or 2 treatments at one year follow-up. The remaining patients had small focal areas left to be treated.
A follow-up appointment will be scheduled by the physician's office to conduct an upper endoscopy to inspect the treated area determine if an additional treatment is necessary.
|
Barrett's Disease
|
Barrett's Oesophagus
|
Barrett's Esophagus
|
Barrett's 0esophagus
|
Barrett's Esophagitis
|
|
Barratts Disease
|
Barratts Oesophagus
|
Barretts Esophagus
|
Barretts 0esophagus
|
Oesophageal Cancer
|
|

